- Low White Blood Cell Count Autoimmune Disorders
- Intermittent Fasting And Immune System Rejuvenation
- White Blood Cells: Function, Ranges, Types, And More
- Interpretation Of The Full Blood Count
- Best Remedies To Increase White Blood Cell Count At Home
- High White Blood Cell Count In The Elderly: Learn Today!
- Dangers Of High & Low White Blood Cells + Underlying Factors
Low White Blood Cell Count Autoimmune Disorders – Don’t miss our biggest sale of the year, save 60% on ALL plans! Sale ends November 27th at 11:59 PM PT.
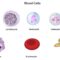
Granulocytosis occurs when a person has too many granulocytes, which are a category of white blood cells in the blood. Granulocytes are characterized by the presence of granules, or small particles, which improve their function. They can be further classified as mast cells, neutrophils, eosinophils and basophils. However, when granulocytosis is discussed, it is usually associated with an increase in neutrophils, eosinophils, or basophils.
Low White Blood Cell Count Autoimmune Disorders

Granulocytes help the immune system fight foreign invaders – such as viruses, bacteria, parasites and fungi – that cause infection or inflammation. Neutrophils play a major role in fighting bacterial infections; eosinophils play a major role in the fight against parasites; and basophils and mast cells play a major role in allergic reactions. Granulocytes develop in the bone marrow, which is the spongy substance inside the bone, and after entering the blood, they respond to signals sent by the immune system. When they come into contact with foreign substances that invade the body, granulocytes undergo degranulation, in which they secrete their specific granules in an attempt to fight off the invaders.
Intermittent Fasting And Immune System Rejuvenation
Granulocytosis can be caused by bone marrow disorders and can also be seen in association with infections and autoimmune disorders.
Most often, granulocytosis is caused by bone marrow disorders that cause an increase in the number of granulocytes produced in the marrow. One of the most common bone marrow disorders resulting in granulocytosis is chronic myeloid leukemia, a cancer of the white blood cells. Other bone marrow-related disorders that can lead to granulocytosis include polycythemia vera (causing an increase in red blood cells), primary myelofibrosis (causing destruction of the bone marrow and consequent scarring of the bone marrow), and essential thrombocythemia (causing an increase in platelets). ).
Infections, especially those caused by bacteria, can also cause granulocytosis. Such cases are the result of the body’s natural immune response to fight infection; as more neutrophils are produced to attack the bacteria, granulocytosis may occur.
Finally, autoimmune disorders, such as rheumatoid arthritis, can also lead to granulocytosis. Individuals with rheumatoid arthritis generally have chronic joint inflammation that can often lead to an increased amount of circulating granulocytes.
White Blood Cells: Function, Ranges, Types, And More
The signs and symptoms of granulocytosis depend on the underlying cause. If it is the result of chronic myeloid leukemia, common signs and symptoms include abnormal bleeding, fatigue, loss of appetite, pale skin, night sweats, and frequent infections. In cases of granulocytosis associated with rheumatoid arthritis, common signs and symptoms include joint pain, swelling, and stiffness. If associated with a bacterial infection, common signs and symptoms include fever, fatigue, headache, nausea, and vomiting.
Granulocytosis is most commonly diagnosed with a blood test called a complete blood count (CBC). A CBC measures the amount of red blood cells, white blood cells, and platelets in an individual’s blood. An elevated white blood cell count may indicate granulocytosis, as well as an underlying disorder, disease, or infection. Similarly, elevated red blood cells or platelets may indicate polycythemia vera or essential thrombocythemia, respectively.
Treatment for granulocytosis is usually aimed at treating the underlying cause. Treatment of the existing condition should help reduce the number of white blood cells in the blood and resolve the granulocytosis.

Granulocytosis occurs when there is an increase in the number of granulocytes (eg, neutrophils, basophils, or eosinophils) in the blood. Granulocytosis is usually a symptom of an underlying condition or disease, especially bacterial infections, autoimmune disorders, or bone marrow disorders. Diagnosis involves a complete blood count and treatment is aimed at mediating the underlying cause. Blood cell disorders are conditions that affect any of your blood cells – these are your red and white blood cells and even platelets. All of these cells form in your bone marrow. While some disorders interfere with the function of one of these cells, they can also damage multiple blood cells and their given function. .
Interpretation Of The Full Blood Count
Below are some common benign blood conditions that affect one’s blood cells and platelets. To help our patients better understand each condition, we’ve included the symptoms, risk factors, ways of diagnosis, and treatment options for each of these benign blood conditions.
What is anemia? Anemia is a blood cell disorder that affects the function of your red blood cells. If you suffer from anemia, your body lacks the healthy blood cells needed to carry oxygen to the rest of the body. Anemia is also sometimes called low hemoglobin. .
The signs and symptoms associated with anemia depend on the severity and type of anemia you have been diagnosed with. In addition, anemia can sometimes manifest itself without symptoms. However, some symptoms that may indicate anemia include:
Anemia is often associated with a lack of certain vitamins and minerals, chronic conditions and intestinal disorders. Additionally, other risk factors for anemia include pregnancy, menstruation, age, and a family history of anemia.
Best Remedies To Increase White Blood Cell Count At Home
To diagnose anemia, our hematologists may recommend a full blood count (FBC), which will tell us the level of red blood cells present in your blood.
If this is due to a dietary deficiency, supplementation with deficient nutrients (folate, iron or vitamin B12) may be adequate. If there are other causes, treatment will need to be directed accordingly.
Iron deficiency anemia is a common form of anemia when the body does not have enough iron to produce hemoglobin.

Some common symptoms of iron deficiency anemia are general fatigue, unusual weakness, pale skin, burning sensation in the legs, swelling and pain in the tongue, brittle nails and frequent headaches.
High White Blood Cell Count In The Elderly: Learn Today!
Iron deficiency anemia usually results from low dietary intake, blood loss, increased iron requirements during pregnancy, and decreased dietary iron absorption. Risk factors for iron deficiency include age, genetic conditions, and lifestyle choices.
Our hematologists can recommend a series of tests to diagnose iron deficiency anemia. These tests may include a full blood count (FBC), an iron profile, and additional diagnostic tests such as a colonoscopy and endoscopy may be needed to rule out any bowel causes.
Treatment options for iron deficiency anemia may include oral iron supplements, intravenous iron infusion, and red blood cell transfusions.
More information about iron deficiency anemia, its symptoms, risk factors and treatment options can be found here.
White Blood Cell Count Profiles In Multiple Sclerosis During Attacks Before The Initiation Of Acute And Chronic Treatments
Aplastic anemia is a rare and serious condition in which the body produces inadequate blood cells. This causes the body to feel tired and can increase the risk of uncontrolled bleeding and infections.
Some risk factors for aplastic anemia include exposure to toxic chemicals, radiation or chemotherapy to treat cancer, certain prescription drugs, pregnancy, and autoimmune disorders.
Treatment of aplastic anemia depends on the age and severity of the patient’s condition. The treatment aims to restore the production of blood cells. It may resolve spontaneously without treatment if the condition is mild, although this is not common. Patients will likely need blood and platelet transfusions to prevent and control infections.

Thalassemia is a genetic blood disorder that affects the production of red blood cells. Abnormal blood production means that affected individuals do not make adequate amounts of functional red blood cells.
An Ultimate Cbc Test Cheat Sheet You Should Check
There are several types of thalassemia, the most common forms being alpha and beta thalassemia. Clinically, patients with thalassemia may have thalassemia minor or thalassemia major.
Symptoms of thalassemia can vary, with some people having no visible symptoms, while others develop symptoms later in adolescence. Some of the more common symptoms include:
To diagnose thalassemia, our hematologists may recommend a full blood count (FBC). More specific blood tests such as hemoglobin electrophoresis and red blood cell genotyping are needed to clarify the diagnosis of thalassemia and determine the thalassemia subgroup.
Depending on the type of thalassemia you are diagnosed with, treatment options may vary – some forms of thalassemia do not require treatment. However, if you need treatment, our hematologists may recommend iron chelation, blood transfusion, bone marrow or blood stem cell transplantation.
Dangers Of High & Low White Blood Cells + Underlying Factors
Deep vein thrombosis (DVT) is a blood condition in which a blood clot (thrombus) forms in a blood vessel located deep in the body, usually in the leg or arm. This leads to a complete or partial blockage of blood flow through the vein, causing the affected limb to become painful, red and swollen.
Various risk factors increase your chances of developing deep vein thrombosis. These include prolonged bed rest or prolonged sitting, age, being overweight, smoking, cancer, heart failure, genetics, birth control pills, and pregnancy.
Ultrasound is commonly used in the diagnosis of deep vein thrombosis. It allows our hematologists to check that your blood is flowing normally through your veins.

The recommended treatment is an anticoagulant, a drug that will thin the blood and prevent the clot from getting bigger and preventing it from breaking off and causing a pulmonary embolism. The blood clot will naturally dissolve in your body over time.
Is High Wbc (white Blood Cells) Count In Pregnancy Harmful?
Pulmonary embolism refers to a condition in which a blood clot (thrombus) is lodged in the blood vessels of the lungs. PE usually begins as a clot in the deep veins (also known as deep vein thrombosis or DVT) in the leg that has become detached
Low white blood cell disorders, autoimmune disorders that cause high white blood cell count, autoimmune disease causes low white blood cell count, high white blood cell count autoimmune, high white blood cell count autoimmune diseases, autoimmune disorders that cause low white blood cell count, hiv and low white blood cell count, what autoimmune disease causes low white blood cell count, low white blood cell count autoimmune, blood disorders low white cell count, leukemia low white blood cell count, what autoimmune disorders cause low white blood cell count